On August, 3 2020, the Centers for Medicare & Medicaid Services (CMS) issued a proposed rule that announced and solicited public comments on proposed policy changes for Medicare payments under the Physician Fee Schedule (PFS), and other Medicare Part B issues, on or after January 1, 2021.
With the budget neutrality adjustment to account for changes in relative value units (RVUs), as required by law, the proposed CY 2021 PFS conversion factor has been set to $32.26, a decrease of $3.83 from the CY 2020 PFS conversion factor of $36.09. This amounts to a 10.62% decrease.
Chief among the rule’s proposals is an increase in RVUs – and reimbursement – for primary care services and chronic care disease management. However, to offset the changes to RVUs for these services, the rule also includes a reduction in the payment conversion factor.
The reduction would account for the budget neutrality adjustment for changes in RVUs as required by law. This would likely have the largest impact on specialists, including their procedures as well as diagnostic and ancillary service CPT codes.
While providers are generally supportive of increased investments in primary care and chronic disease management, the reduction would likely result in a material percentage cut to physician payment in 2021.
As stated by the AMA, “Payment reductions of this magnitude would be a major problem at any time, but to impose cuts of this magnitude during or immediately after the COVID-19 pandemic, including steep cuts to many of the specialties that have been on the front lines in efforts to treat patients in places with widespread infection, is unconscionable.”
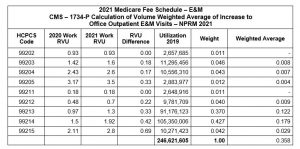
Table A below shows the overall proposed changes to the WRVU values for the 2021 Medicare Fee Schedule as compared to the current 2020 WRVU values and their related weighted average differences. The impact has the potential to be significant when you view it from a big-picture perspective, as we describe in Table B below.
Table A:
As demonstrated by provider feedback, the Medicare Physician Fee Schedule has a wide reach and will significantly impact physician reimbursement. Since most commercial payors’ fee schedules follow Medicare, the effect on these changes could likely impact a group’s total reimbursement in a material fashion.
We built an analysis to see what the overall impacts could be on our clients who have multiple subspecialities (shown below).
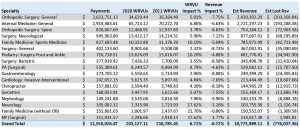
Table B:
As seen in Table B, this group’s overall summary is showing around a 6.72% WRVU impact compared to the 2020 WRVUs. The data from the table is also showing us that if the projected revenue impact is based on these same volumes, 2021 CMS reimbursement will have an overall decrease of 6.72% compared to 2020 CMS reimbursement. The ranges on the WRVU impact by specialty varied anywhere between approximately 3% and 27%, while the estimated revenue impact was anywhere between a negative 1% up to a negative impact of 9%. We believe that this analysis is a good indication of what could be expected if no material changes are made by CMS.
While concerns with the proposed rule for 2021 are equally wide-reaching, and significant comments and possible revisions are expected before the fee schedule is finalized prior to the end of 2020, we believe that CMS should consider the impact COVID-19 has had on providers before finalizing the fee schedule.
As groups and health systems complete their 2021 budgeting, we recommend they take a deeper look at the possible impact that this new fee schedule may have.
Ronnen Isakov is Managing Director Advisory Service of MMG Healthcare Solutions / Medic Management Group. His background includes extensive work in areas including business advisory, valuation, network optimization, transaction support, and project management. MMG is a national provider of consulting services and back office administrative support to independent and system owned physician practice groups. Additionally, MMG has been formally recognized as a multi-year Northeast Ohio Top Workplaces award winner.